In the modern world, the resonance of this disease with cervical osteochondrosis cannot be underestimated. Osteochondrosis is more common in the cervical region than in other vertebral regions. Almost all people over the age of 25 suffer from this disorder to some extent.

The occurrence of cervical osteochondrosis is mainly due to a sedentary lifestyle, especially the historical transition of people from manual to mental work, albeit to a moderate degree, accompanied by sitting work.
Cervical osteochondrosis is a degenerative dystrophic disease of the cervical spine that causes disc damage, which is common in osteochondrosis. Since this part of the spine is very flexible in nature, but at the same time vulnerable due to the dysplasia of the muscular corset, any negative impact on the neck or back will first affect the neck area. Since degenerative changes occur most often in the most active parts of the vertebral body, it is the nerve endings at the level of C5. . . C7 that are most often affected in the cervical region.
Because the symptoms of cervical osteochondrosis are controversial, they are not always considered symptoms of the disease, which often leads to seeking help from specialists in other medical fields. Let's consider them in more detail.
symptom
Due to the compactness of the cervical spine, compared to other departments, even slight tension in the neck muscles or displacement of the cervical vertebrae can cause compression or pinching of the nerve roots and also affect vessels located in this department. Well, osteophytes - bone growths, called "salt deposits" in folk remedies, and formed under conditions of the development of cervical osteochondrosis diseases, as a result, lead to a significant deterioration in the course of the disease.
The clinical manifestations of cervical osteochondrosis, that is, its symptoms, can be divided into reflex symptoms and radicular symptoms of cervical osteochondrosis.
Reflex symptoms of cervical osteochondrosis
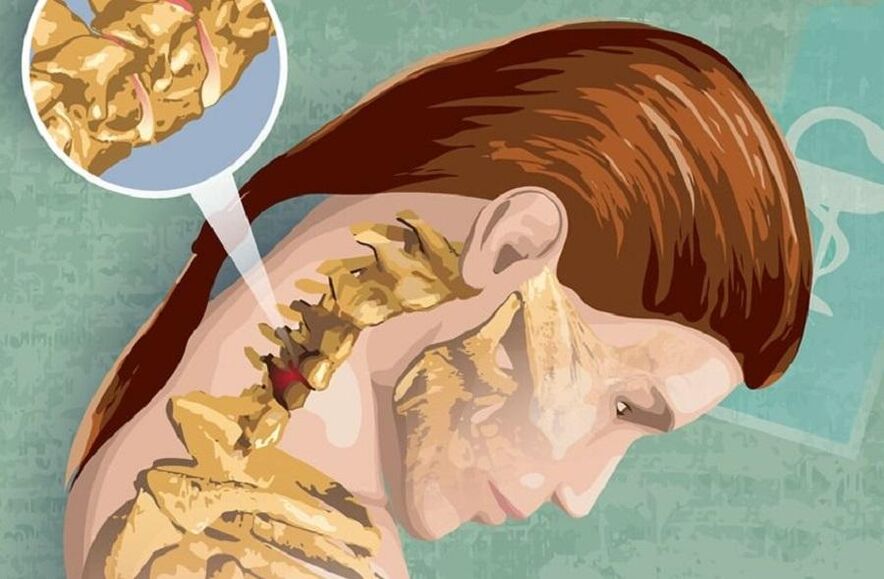
Reflex symptoms of cervical osteochondrosis include so-called "low back pain", which is characterized by severe, severe pain in the neck that is markedly intensified with any exercise. For this reason, patients often assume some forced, most comfortable head position. In addition, the typical "crunch" is likely to occur during turning or other head movements.
With cervical osteochondrosis, patients often experience pressure headaches that radiate to the eyeball or the temporal portion of the head. Also, sometimes at the same time, the sharpness of visual perception may decrease, as if "everything is in sight".
Vertebral artery syndrome can also develop when its nerve plexus is stimulated, which is often misdiagnosed as disruption of blood circulation to the brain due to the patient's dizziness. Symptoms of this cervical osteochondrosis can manifest as sudden head movements with nausea and possible vomiting.
In addition to the above, reflex symptoms of cervical osteochondrosis include heart disease syndrome, in which there is a feeling similar to an angina pectoris attack. But the presentation of the symptoms of this osteochondrosis is often combined with the complexity of other symptoms of the disease, so it usually does not cause difficulties in making a correct diagnosis.
Nerve root symptoms in cervical osteochondrosis
The radicular symptoms of cervical osteochondrosis usually occur due to compression of the spinal nerve endings - the roots. In this case, the sensory disturbances affecting motor function depend entirely on the specific nerve root that is injured, namely:
- C1 - decreased sensitivity in the back of the head;
- C2 - the occurrence of pain in the parietal or occipital region of the head;
- C3 - Violation of sensitivity and appearance of neck pain, injury to the spinal cord, most likely a violation of speech function due to loss of sensitivity and control of the tongue;
- C4 - Pain and decreased sensitivity in the dorsal region of the scapula, and pain in the heart and liver regions, along with decreased neck muscle tone and possible respiratory disturbances;
- C5 - decreased sensitivity and pain in the outer shoulder surface;
- C6 - Pain radiating from the neck area to the scapula, outer surface of the shoulder, forearm, and from the wrist to the thumb;
- C7 - same pain as C6, but radiating from the scapula to the back surface of the shoulder and further from the forearm to the 2nd to 4th fingers, the pain area is less sensitive;
- C8 - Decreased sensitivity and pain from neck to shoulder, then forearm to pinky.
treat
Cervical osteochondrosis is a rather complex and extremely unpleasant disease whose treatment requires consistency, duration and phase. Therapeutic treatment of cervical osteochondrosis begins with the complete cessation of painful symptoms of cervical osteochondrosis and the elimination of inflammation in the region of the neck affected by the disease.
During the treatment of cervical osteochondrosis, patients use classic analgesics, such as metabolites, ketolosan, or balagin. Although NSAIDs have recently been widely used in the treatment of cervical osteochondrosis, they can effectively relieve pain and reduce inflammatory activity.
Among other things, in the treatment of osteochondrosis of the cervical spine, chondroprotective agents are used, which slow down the process of destruction of cartilage tissues and, according to many experts, also help their regeneration process. In addition, patients are prescribed B vitamins, which improve metabolic processes in the patient's body.
Using topical gels or ointments for cervical osteochondrosis isn't effective, but it makes sense because of the extra massaging of the cervical area of the spine during the process of rubbing them into the skin.
Physiotherapy procedures are also combined with traditional cervical osteochondrosis medication, especially the use of magnetic therapy through special medical equipment well-known among specialists and patients is particularly effective. In addition to the above, therapeutic massage, physiotherapy exercises and manual therapy are used. However, in particularly severe cases, surgical intervention may also be required.
Prevention of cervical osteochondrosis
On its own, preventing cervical osteochondrosis is not difficult. recommended:
- maintain an active and healthy lifestyle,
- exercise, or at least morning exercise,
- the competent organisation of the workplace,
- observe the work and rest regime,
- During long hours of work in a seated position - During working hours, warm up several times and ensure the correct position of the head and posture during the work.
It is also important to choose a comfortable pillow and mattress to sleep in. But for those who already suffer from this condition, daily use of specialized orthopaedic products for a restful night's sleep is highly recommended.
























